Op ed: To avoid future public health crises, we must address the collateral damage of COVID-19
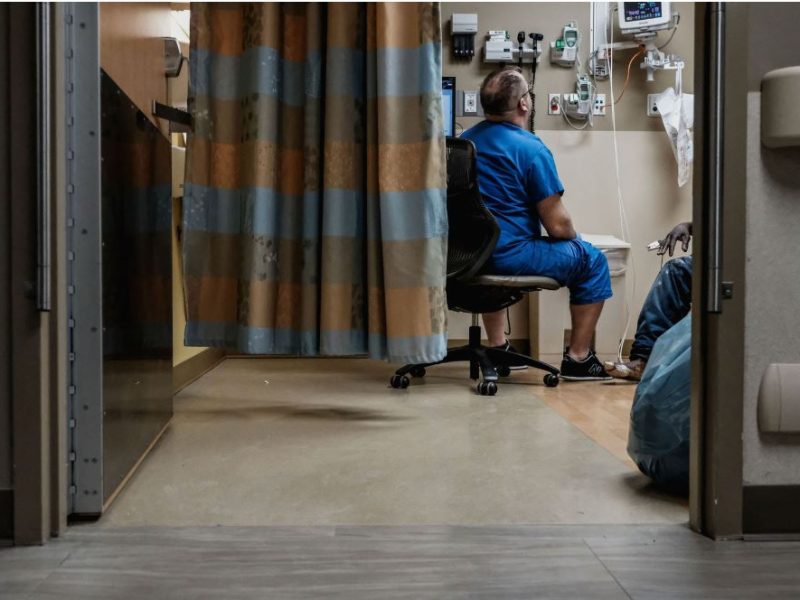
Athletes are continuously told to “keep your eye on the ball” as if concentration is the magic ingredient to winning. But if you have ever played or watched a sport, you know that there is much more to winning than just keeping your eye on the ball. In our response to COVID-19, we risk other emerging crises as well as excess illness and death due to non-COVID related disease if we solely focus on the COVID pandemic.
There are multiple secondary effects of the COVID-19 pandemic that could create a cascade of future public health crises and further health disparities once this pandemic is over. I have personally lost three family members in the past 3 weeks. The first died as a result of COVID-19. The second suffered at home for fear of contracting coronavirus, and by the time she went to the hospital, it was too late. The third, went to the hospital during the pandemic for a pre-existing health condition and died alone in her hospital room. Each of these deaths point to several problems that we as a nation must address while we fight this pandemic.
First, we must address the ongoing psychological and mental trauma that people are facing due to job loss, living in fear, being socially and physically isolated, and witnessing death on an unparalleled scale during this pandemic. The mental and emotional health of our nation is as important as our physical health. Mental illness can be difficult to recognize and harder to treat than say a broken leg, but we have a system of care and good evidence that mental health is manageable and mental illness is treatable. It is safe to assume that the mental health needs of our nation have increased during this pandemic for a multitude of reasons and it is imperative that we expand our system of care to meet these increased needs.
Second, we must ensure that accurate and timely information is made available to the community at-large about how best to manage non-COVID related illness in the midst of this crisis. The life-saving stroke medication known as “clot buster” is only an option if administered within the first several hours of the onset of a stroke. In the stroke community, they say ‘time is brain’; the longer people wait to go the hospital, the more neurons (brain cells) die. Researchers have documented a 39% decrease in hospital imaging for stroke in the first 2 months following the COVID-19 pandemic. Delays in the treatment of medical conditions like stroke and other chronic conditions due to fear of leaving the house or going to the hospital, will result in excess preventable illness and death from these conditions.
Third, we must also promote the ongoing practice of primary and preventive care. As an example, children need to continue to receive well child visits and vaccinations. Local hospital partners have reported significant decreases in well child visits and the CDC reports significant reductions in pediatric vaccine ordering after the COVID-19 emergency declaration. If we lose sight of the need for these basic preventive and primary care services, we could see the outbreak of diseases like measles which, according to the CDC spiked in 2019 in primarily underimmunized populations and threated the eradication of the disease. We also need to continue routine screenings for diseases like breast cancer and colorectal cancer, which have the best prognosis when detected and treated early. The gaps in primary and preventive care will predictably have a greater impact on vulnerable populations that already have difficulty accessing preventive services and screening.
Lastly, we must deal with health inequities, that is the systematic unfairness that prevents assurance of the condition of optimal health for all people. During COVID-19, this includes fair access to personal protective equipment, testing, health care, and treatment – despite race, age, gender, health status, incarceration status, or whether someone has health insurance or a pre-existing health condition. It is well documented that COVID-19 has disproportionately impacted African Americans. The racial disparities in health that we have seen during this pandemic however, pre-date the introduction of the SARS-CoV-2 virus and merit our immediate and deliberate attention and mitigation – including after this pandemic is over.
As we keep our eye on the ball of COVID-19, we must not simultaneously lose sight of good public health practices, the need for primary and preventive care, and other emerging physical and mental health needs. To do so will only further exacerbate non-COVID related death, disability and disparities and give way to avoidable future public health crises. If we take a step back and get a bird’s-eye view of the whole game, we can intervene on the direct and collateral effects of COVID-19, and position ourselves to come out of this pandemic better than we went in.
Debra Furr-Holden, PhD is the Associate Dean for Public Health Integration at Michigan State University College of Human Medicine.
Support local news!
Flint Beat is here to empower, impact and inform our community. Show your support today!
Choose a monthly amount
Basic
Standard
Pro
Custom Amount
Thank you for your support!