With Medicaid eligibility evaluations set to resume, officials advise Flint residents on how to prepare

Flint, MI—The state of Michigan will soon resume checking enrollee’s eligibility for Medicaid, and officials are advising Flint and Genesee County residents to get prepared.
After putting the process on pause during the COVID-19 pandemic, the state is restarting annual Medicaid eligibility redeterminations in April 2023.
To avoid risk of losing coverage, James Milanowski, president and CEO of the Genesee Health Plan, advises people currently enrolled in Medicaid to ensure that their basic information is up to date.
“The most important thing people can do that have Medicaid is make sure their most current address and phone number are on file with the state,” Milanowski said. “That’s really the big message right now.”
The pause on eligibility check-ins came courtesy of the Families First Coronavirus Response Act, passed in March 2020, which required states to continue Medicaid coverage for most beneficiaries without requiring annual reevaluations. But new legislation, signed in December 2022, ends beneficiaries’ continuous enrollment on March 31, 2023.
Yaushica Aubert, president and CEO of the Valley Area Agency On Aging in Flint, said the expiring continuous enrollment provision offered individuals health coverage when they may not have qualified for Medicaid otherwise, helping them avoid out-of-pocket insurance costs from private insurance.
Medicaid coverage, she added, is a critical lifeline for many people in Flint, where over 35% of the population lives in poverty according to recent Census data.
“A lot of people in Flint are underinsured or not insured,” Aubert said. “Medicaid has been that sole source of insurance, especially during this time with the pandemic and flu and other outbreaks. Being able to have medical insurance to help cover doctor’s visits, hospital visits and medications has been extremely important.”
According to the Kaiser Family Foundation, Medicaid enrollment grew significantly, by and large, due to the continuous enrollment provision.
In Genesee County, the number of Medicaid recipients jumped to 170,005 from 136,619 between March 2020 and January 2023, according to data from the Michigan Department of Health and Human Services (MDHHS). Overall, Medicaid beneficiaries in Michigan increased by more than 736,500 over the same time period.
Milanowski said continuous enrollment has also helped people retain health coverage during the COVID public health emergency.
“They might have lost their jobs and lost their health care benefits, and so this continuous enrollment has kept many people able to see their doctor or get prescriptions or any other care that they might need,” he said.
While the number of people who will no longer qualify for Medicaid is currently unclear, according to Bob Wheaton, public information officer at MDHHS, local officials note that they do expect thousands to be affected by the reevaluations.
For the Genesee Health Plan, which provides health coverage for uninsured Genesee County residents, Milanowski estimates that the number of its beneficiaries will increase anywhere from 3,000 to 5,000 as Medicaid redeterminations resume.
“During this time with the rise of people getting Medicaid, there were more people on Medicaid and less people on the Genesee Health Plan,” Milanowski said. “We expect more of those people to come to us and we’ll cover them while they’re applying, or maybe they don’t qualify … anymore, and we can provide some type of health care coverage to them.”
Meanwhile, Farah Hanley, chief deputy director for health at MDHHS, said current Medicaid recipients with a June 2023 renewal month will be first to be reevaluated for eligibility. She noted that MDHHS will start “passive redeterminations”—or processing beneficiaries’ redeterminations without additional information—for that cohort in April.
“Those individuals will not have to go in and actually apply, because they will be passively renewed based on eligibility for other programs,” Hanley said.
Other programs may mean Social Security Disability Insurance or food assistance, for example, Wheaton added.
For those whose Medicaid benefits are not passively renewed, Hanley said the state will send redetermination packets to seek more information regarding their eligibility in May, prior to their June renewal month.
“The most important thing to tell someone who’s on Medicaid right now is if in the month of May, they receive a Medicaid redetermination packet from the department, please fill it out and send it back,” Hanley said. “If they get any contact from the department related to whether their address is updated or anything like that, please follow up.”
Below is the complete schedule for Medicaid eligibility redeterminations. Current recipients who otherwise would have had April or May 2023 renewal months will not be affected until 2024, according to Wheaton.
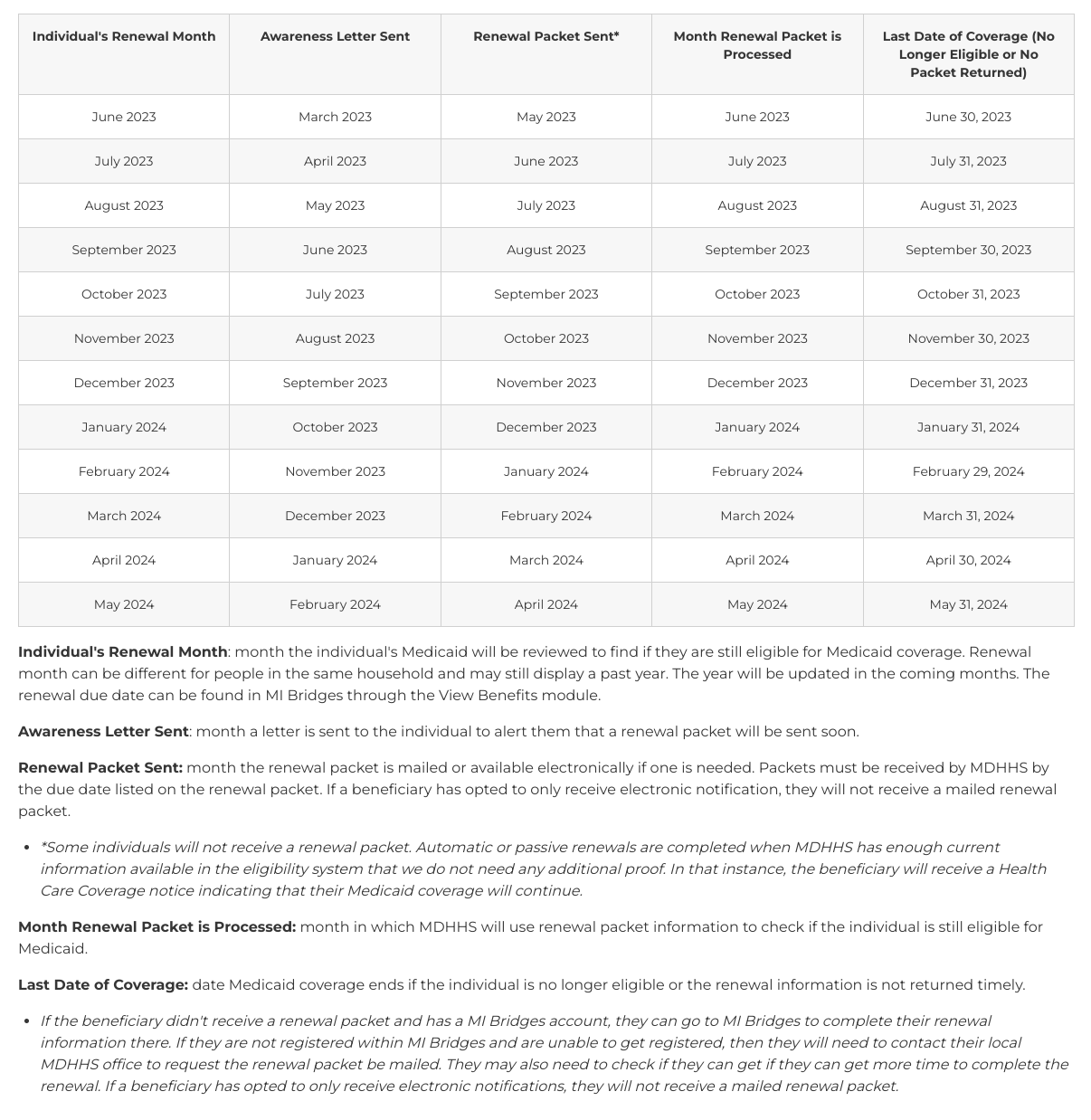
All in all, Hanley said that “as we comply with federal laws and rules, the department is committed to ensuring that coverage for beneficiaries enrolled in Medicaid is maximized to whatever extent possible, and that we have implemented, we believe, a robust process with various safeguards to ensure that that happens.”
The state will also be carrying out outreach efforts to connect residents deemed ineligible, or who lose Medicaid coverage for procedural reasons, with support and resources, according to Erin Emerson, senior policy executive in MDHHS’ Office of Strategic Partnerships and Medicaid Administrative Services.
In Flint and Genesee County specifically, Milanowski said organizations like the Genesee Health Plan, Valley Area Agency On Aging, Greater Flint Health Coalition and Hamilton Community Health Network, will all be able to provide assistance with navigating the Medicaid redetermination process alongside local MDHHS offices.
Support local news!
Flint Beat is here to empower, impact and inform our community. Show your support today!
Choose a monthly amount
Basic
Standard
Pro
Custom Amount
Thank you for your support!